Roadblock: When Mental Health Stigma Prevents Treatment of Physical Pain
It’s a widely known fact that people with mental illness face stigma at school, at work, and even at home. What gets less attention is the difficulty people with mental illness encounter in getting diagnosed with and treated for more visible illnesses. Stigma is a roadblock to treatment. As someone who lives with Bipolar II (diagnosed at 18-yrs old), Polycystic Ovarian Syndrome (19), Myasthenia Gravis (24), and asthma (24), I know stigma.
This brings me today’s WEGO prompt: Invisible Illness vs. Visible Illness : What are some stigmas you have experienced with your invisible OR visible illness that have made you feel invisible? How have you tackled them?
MY ANSWER: “Doctor, it’s not in my head!”
Mental illnesses are a type of invisible illness. When people with diagnosed mental illnesses (like anxiety, depression, bipolar disorder, or panic attacks) see their doctors to get treated for physical pain with tangible symptoms, they are often not taken seriously. I’ve heard countless stories of discrimination from people with Cancer, Multiple Sclerosis, Lupus, Sjogren’s, and Fibromyalgia who sought help upon exhibiting symptoms. In 2008 I experienced
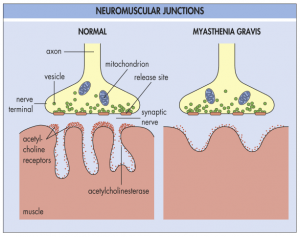
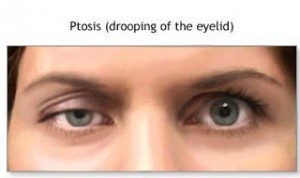
stigma when I tried to get help for Myasthenia Gravis (MG), a neuromuscular autoimmune disease. By September, I had all but one of MG’s symptoms (difficulty breathing); relatives and friends who are doctors call me a “textbook case.” I saw my primary physician twice between August and September of 2008. Let’s call her “Dr. M-Ron.” At my August visit, I told her that I was tired all the time and that I had to manually pull up my eyelids because they kept drooping (ptosis).
Weeks later, when I was climbing up a long flight of stairs at work, I started falling. And falling. I couldn’t get up because I could not feel anything below my waist. I was coaching high school mock trial then. Many students stepped over my body and rushed to class before I successfully begged two students to help me up. I returned to Dr. M-Ron with this information and recalled the multiple times I fell down during yoga. I also told her about how I sometimes couldn’t feel my legs or arms at all. I told her about my problems speaking coherently (which she could see for herself) and trouble swallowing food (dysphasia). What did the doctor tell me? She said, “You’re stressed out.” I knew this woman had flipped. I told her, “With all due respect, I’m not stressed or depressed. If this was stress, then millions of Americans should be falling down the stairs at work and school because life is inherently stressful.” A simple blood test would have revealed I had MG but she did not order it. I didn’t take Dr. M-Ron’s words as gospel truth. In October, I saw a neurologist who immediately diagnosed me with MG after examining me. The neuro also ordered a blood test, which decisively confirmed MG.
Critical Condition
On October 10th, just four days after I was diagnosed with MG, I was already in Myasthenic Crisis and hospitalized for two weeks. By that point, I was too weak to breathe, feed myself, and bathe myself—all consequences of the late diagnosis. When I obtained Dr. M-Ron’s notes from my visits, I learned that she wrote, “Patient has Multiple Sclerosis, Miesthenia Gravis, or stress?” (Yes, she did not know how to spell this illness!) Again, despite any suspicions, Dr. M-Ron never ordered the test. I reported her negligence to the insurance company. Sadly she was not the only doctor who gave me a hard time just because I have bipolar disorder. Basically, stigma almost killed me.
Today I have physicians that listen to me. Since 2009, I’ve had a fantastic neurologist who is a renowned expert on Myasthenia Gravis (and Sjogren’s). Here are some lessons I learned.
Tips for Dealing with Stigma:
- Persevere: Some people are just awful (I want to use another word here but my mother reads this blog). We can’t change everyone. Reasoning with doctors who had stigma (including one from a famous clinic) has never worked for me. If a doctor doesn’t respect you, find someone who does. (Yes, I know it’s easier said than done.) I have improved with MG because my neurologist of four years actually listens to patients. She graduated summa cum laude from a prestigious medical school but she has no “God Complex.”
- Be Discriminating in Sharing Mental Health History: I talk about my bipolar disorder when I see my therapist—seeing her is maintenance, which is part of why my bipolar disorder is under control. When I saw an ENT (Ears, Nose, Throat Specialist) this summer because of problems with my nose and ears, I didn’t discuss my bipolar disorder because it was irrelevant. By contrast, we talked a lot about MG, which was relevant. I got a swift diagnosis. Without it, I might be deaf now.
Have you ever faced stigma? Stay tuned for tomorrow as we continue WEGO’s November Health Blog Post Month. I will also do more blogging about mental illness.
Good News!
Fashionably ill has recently been nominated for a WEGO: Best in Show Blog Award. I’ve also been nominated for Health Activist Hero. You can endorse me for both awards here on WEGO’s website (endorsing is like voting; no money required–click purple button twice).
–Your Stylist, Jessica Gimeno
Like Fashionably ill on Facebook
Meet other warriors! “Like” us on Facebook at https://www.facebook.com/fashionablyill.






This post is one in which a large number of people will definitely relate to you. My neurological condition was undiagnosed for years because the doctors had previously diagnosed me with an anxiety disorder and consequently put down all of my symptoms down to the psychiatric diagnosis. It truly makes you wonder how many people who have labelled as having a psychiatric condition are actually living with a physical condition.
Great post!! xx
I was just wondering how you handle medical charts. I don’t talk about either the actual conditions I have that keep me from getting diagnosed and treated (OCD and PTSD) or the ones that while very serious and real I’ve never actually had (anorexia) but I’m not always able to keep the charts that have that information on them away from new doctors either because I’m not always allowed to self refer or the doctor refuses to see me without first seeing my records.
What a great question! Yes sometimes a new doctor doesn’t care and sometimes they do. One thing that helps me is having a “calm face” when someone inappropriately brings up the bipolar disorder and I’m supposed to be treated for my autoimmune disease or some physical problem. I’ve learned to look *unfazed.* When people say something usually (“I’m surprised. You don’t look bipolar”), I say “I have this disease but it hardly defines me much like my race or color of my skin. I don’t think about these things every day.” That usually eases the tension. That being said, if someone is determined to be a bigot (and discriminate against someone with a diagnosed mental illness), the best thing to do is leave and find another doctor (though that can be tiring).
I’m shaking just reading this. I have written about myself and discussed this many times. I live this regularly. I once went into an ER covered in hives only to be put in m.i. scrubs. Doc came in, asked why. I shrugged and said I’ve learned not to argue so I don’t seem combative. He asked the nurse, she said that I had bipolar, he replied, she has HIVES. Only then did I get the epi and prednisone I needed.
If you are too sunshiney, you are manic, if you disagree too much, combative, if you get annoyed or angry, possibly dangerous, if sad, afraid or disappointing ,you’re depressed…I’ve learned to go in with a flat affect or a small smile and keep it no matter the diagnosis or information given. It was kinda tough with some of the rotten diagnosis, too.
I could continue with the stories. I have three rare issues. I am only now after YEARS of diligence getting one or two doctors to even begin to look at my serious condition. Even with the seriousness, I still get blown off by many. I am simply a number. They go home and sleep if I die tomorrow.
What happens to those with mental illnesses so grave they can’t advocate for themselves? I shudder.
Thanks for a great post. These are terrific tips and I’m so glad you didn’t give up, that, thank GOD, they gave you a diagnosis in time and we have you here to educate us.
ok, yeah. This is a pretty epic post.
Dear Liz,
Thanks for the feedback. Spreading awareness about stigma is something we can do together. Bless you,
Yes, yes, yes! Interestingly enough, even WITHOUT that type of diagnosis, so many doctors dismiss and disregard patient complaints.
For years, I went from doctor to doctor, trying to get diagnosed (and treated). I knew that I had Fibromyalgia – I fit all the criteria, had all the symptoms (and most of the other conditions with comorbidity). Still, internists, rheumatologists, neurologists, and more … in all, I saw 12 different doctors, and most simply said “oh, maybe you’re just depressed.” So my symptoms didn’t matter … I didn’t matter.
Sometime after that, I was listening to the radio, and John Tesh (of all people) said something I’ll never forget. Basically, it was a reminder that when you go to a doctor, you’re hiring that person to work for you. So if you’re not satisfied with the work, fire them and find someone else. In hindsight, that makes perfect sense … but at the time, it was a world-changing revelation!
Until then, I’d felt like I was at the mercy of the doctors, and if they didn’t take me seriously, then I would just continue to suffer. With those words, though, I was empowered! Since then, I’ve found a whole new set of doctors who listen to me, believe me, and care about helping me. I’ve been diagnosed with fibromyalgia, rheumatoid arthritis, hypothyroidism (due to an autoimmune thyroid condition), and a few other things. They recommended that I see a therapist, but not because “it’s all in my head.” They realize that living with chronic (though invisible) debilitating illnesses is immensely stressful, and thought it would help for me to have someone to talk to about it, who could maybe help me develop coping mechanisms, etc. They recognize that (as Hugh Laurie stated in my favorite line ever from House) “I’m not in pain because I’m depressed … I’m depressed because I’m in pain.” It’s a world of difference!
Good info. Lucky me I discovered your website by chance (stumbleupon).
I’ve book-marked it for later!
Great! I’m happy to hear that. I just uploaded my TEDx Talk on depression (it’s in the BIO section and newest post in BLOG section). I hope you like it. Blessings, Jessica
Great blog, so glad you persevered despite the stupidity of your original doctor. God bless you. You are also beautiful. Thanks for sharing your experience. My GP was a jerk, as well.
Thank you! You are so kind. Perseverance is important; thanks for sharing your similar experience. God bless you too 🙂